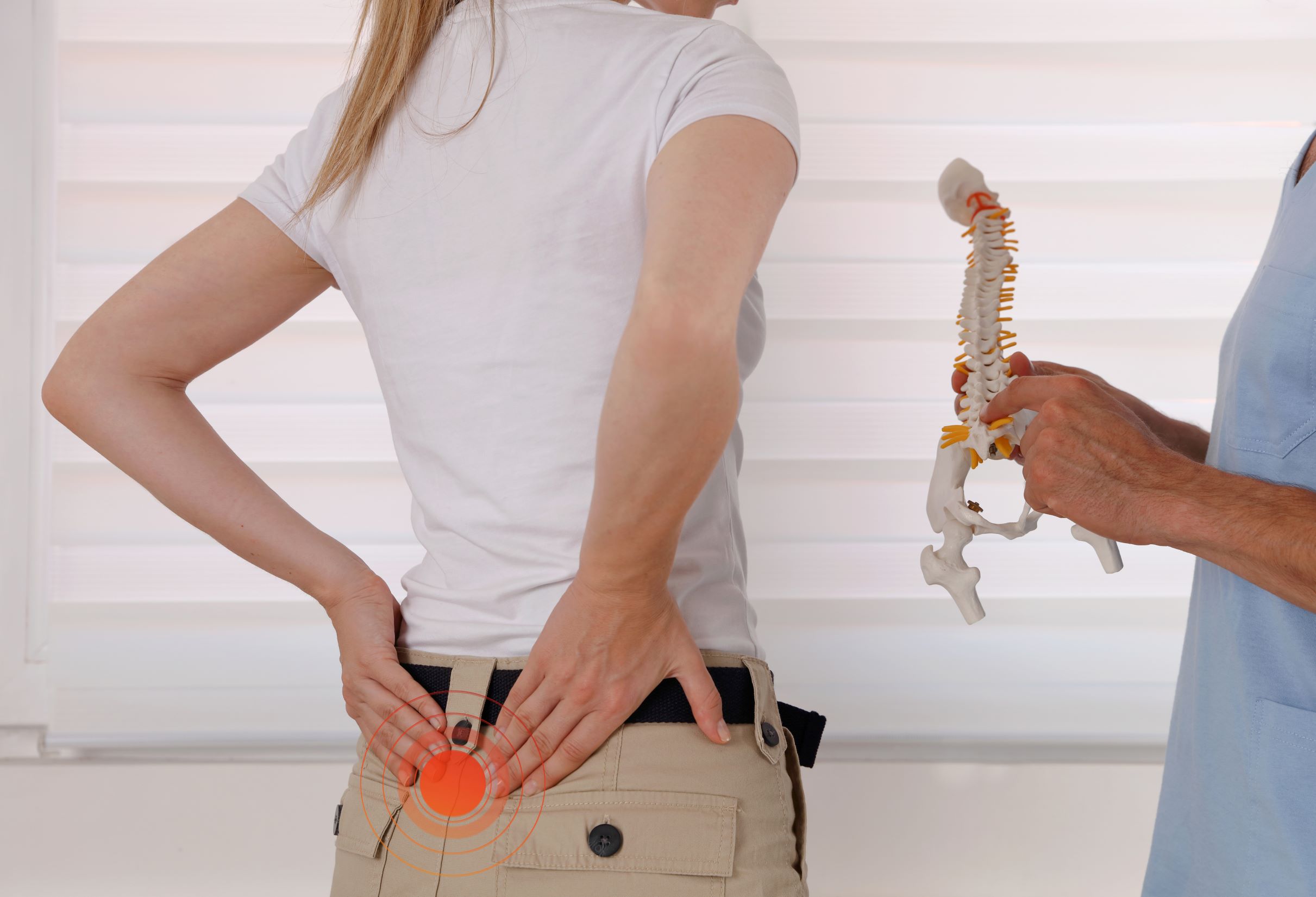
A herniated disc is a common cause of back pain. The discs act as shock absorbers of the spine and are located between each of the vertebrae. A disc becomes herniated when cracks or tears on the outer surface allow fluid from inside the disc to leak out. The nerves around the damaged disc can become compressed and irritated. While a herniated disc can occur anywhere along the spine, the most problematic areas are the cervical spine (neck) and the lumbar spine (low back).
Could a herniated disc be causing your pain?
The pain from a herniated disc often begins suddenly. The patient may not be able to recall a specific injury or event that preceded the pain. The location of symptoms depends on where in the spine the herniation has occurred. Herniated cervical discs typically affect the neck and arms. Herniated discs in the lumbar spine affect the low back, buttocks, and legs.
Cervical herniation
There may be neck pain and stiffness that restricts range of movement. Certain head positions may aggravate the condition. Pain can radiate from the neck into the shoulders and down the arm to the hand and fingers. Numbness and weakness are also common complaints with a cervical disc herniation. Usually only one arm will be affected.
Lumbar herniation
With a lumbar disc herniation, the pain usually becomes worse when sitting. Walking may help to relieve the pain. There is often compression and irritation along the sciatic nerve. Pain can travel down the leg from the buttocks to the foot. Typically, only one leg is affected. As in the cervical herniation, there may be numbness, tingling, and weakness on the affected side. A herniated lumbar disc may be aggravated by specific activities such as bending forward, lifting heavy objects, pushing or pulling things, and coughing or sneezing.
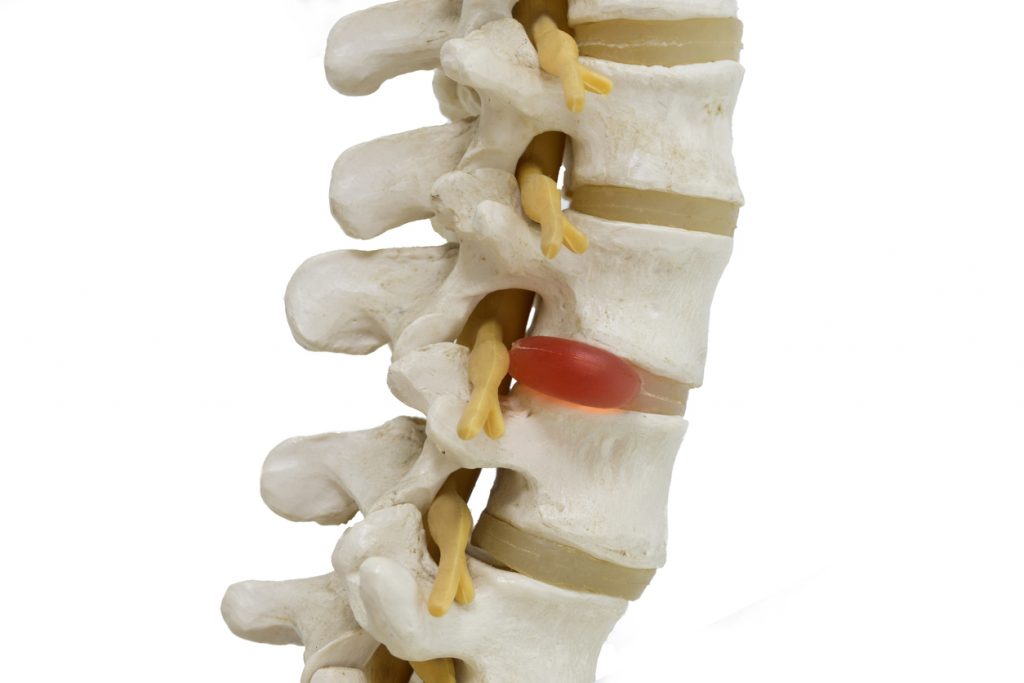
What causes a disc to herniate?
A major factor in disc herniation is age related degenerative disc disease. Spinal discs dry out as we age, and there is not a lot that can be done to prevent it from happening. Normal wear and tear on the discs can cause cracks and small tears on the outer surface, causing fluid to leak from the disc. Arthritis and osteoporosis also contribute to degeneration of spinal discs. Some type of sudden trauma to the spine, such as an accident or fall, may be responsible for causing a herniated disc.
Diagnosis and treatment of a herniated disc
The physician will want to perform a thorough physical examination of the patient. A complete medical history will be reviewed, and the patient will be evaluated for changes in reflexes, muscle weakness, and loss of sensation in the arms or legs. Special diagnostic tests may include a CT scan or MRI. Non-operative treatments may begin with over-the-counter pain relievers to address inflammation and swelling. Physical therapy may include ultrasound, therapeutic exercises, and ice and heat therapies to improve and maintain functional abilities. Interventional pain management, including epidural steroid injections, is another pain relief option. Surgery may be recommended in cases where the pain is severe and non-surgical treatments have not been effective.